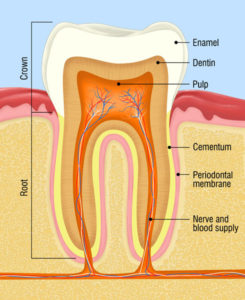
 Root canal therapy, also known as endodontic therapy, is a service necessary due to extensive decay and/or trauma to a tooth that has led to, or will lead to, the death of the nerve (pulp) of the tooth. If untreated, infection and swelling develop resulting in significant pain. Root canal therapy is designed to remove the infected nerve tissue and clean all bacteria from the tooth. The space previously occupied by the nerve tissue is then sealed off to prevent any re-infection of that site. Antibiotics are also typically given to aid the body in ridding itself of the bacteria that has migrated passed the root tips and into the jaw bone.
Root canal therapy, also known as endodontic therapy, is a service necessary due to extensive decay and/or trauma to a tooth that has led to, or will lead to, the death of the nerve (pulp) of the tooth. If untreated, infection and swelling develop resulting in significant pain. Root canal therapy is designed to remove the infected nerve tissue and clean all bacteria from the tooth. The space previously occupied by the nerve tissue is then sealed off to prevent any re-infection of that site. Antibiotics are also typically given to aid the body in ridding itself of the bacteria that has migrated passed the root tips and into the jaw bone.
Treatment may also be necessary when significant restorations or trauma to a tooth cause pulpal damage. Infected pulp can eat away at the surrounding bone area. This is known in dental terminology as an abscess. The individual may feel extreme pain due to this infected pulp. This issue cannot heal on its own, and thus, treatment is required for this situation.
General Symptoms
Infected pulp symptoms may include any of the following: sensitivity to temperatures (hot and cold), sensitivity to sweet foods, sudden swelling, noticeable pain when biting teeth or exerting pressure, or an unpleasant taste coating the mouth. It is not rare that individuals may not experience these symptoms and therefore may not be conscious of a problem until having a dental examination.
Root Canal Procedure
A root canal procedure includes cleaning out the abscess and disinfecting the canals of the tooth. Next, the canals are filled with a special material called gutta percha to create a seal to keep bacteria out. The procedure is often painless due to local anesthetics being implemented. Generally teeth in the front of the mouth take less time than those in the back. An alternative method to root canal therapy is an extraction, or removal of the tooth.
Upon removing the infection, a crown is primarily recommended to keep the tooth that has undergone the root canal from further potential complications and damage.


